- Influenza
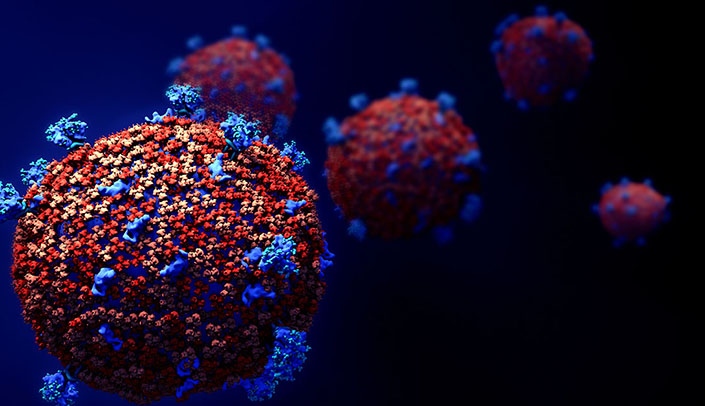
- COVID-19
- Respiratory Syncytial Virus (RSV)
Category: elder care
High blood pressure plus COVID doubles risk of hospital stay.
Even after three COVID-19 vaccine doses, high blood pressure more than doubles the risk for hospitalization with an omicron variant infection.
That’s according to a new study of 912 patients from Cedars-Sinai Medical Center. The researchers analyzed healthsystem data for patients who became infected after receiving three shots. Of the participants, 145 — or nearly 16% — were hospitalized with COVID-19.
Read more at https://www.mcknights.com/news/clinical-news/high-blood-pressure-plus-covid-doubles-risk-of-hospital-stay-study/
World Elder Abuse Awareness Day is June 15th
World Elder Abuse Awareness Day (WEAAD) was launched on June 15, 2006 by the International Network for the Prevention of Elder Abuse and the World Health Organization at the United Nations.
The purpose of WEAAD is to provide an opportunity for communities around the world to promote a better understanding of abuse and neglect of older persons by raising awareness of the cultural, social, economic and demographic processes affecting elder abuse and neglect.
In addition, WEAAD is in support of the United Nations International Plan of Action acknowledging the significance of elder abuse as a public health and human rights issue. WEAAD serves as a call-to-action for individuals, organizations, and communities to raise awareness about elder abuse, neglect, and exploitation.
Visit the WEAAD microsite to learn more https://eldermistreatment.usc.edu/weaad-home/
Long COVID: An Emerging Threat
Long COVID—symptoms that drag on long after someone gets ill with the coronavirus—has many in long term and post-acute care experiencing déjà vu. Diagnostic challenges, questions about treatments, and a limited body of research—these are the same issues they faced at the start of the pandemic over a year ago.
However, while there are still questions, providers have learned much from the pandemic that will help centers navigate the challenges of long COVID and implement and sustain standards, processes, protocols, and interventions that maximize outcomes and quality of life for residents with this condition.
Read more by going to https://bit.ly/3lRAwoq
Online Training to Become Board Certified!
Gero Nurse Prep is an online training course designed to prepare RNs who care for elders to attain board certification in Gerontological Nursing by the American Nurses Credentialing Center (ANCC). This course equips RNs with a broad array of clinical knowledge, skills and competencies that are tested on the ANCC certification exam and essential for quality gerontological nursing practice and leadership of elder care teams.
To find out more:
Watch this short video https://www.youtube.com/watch?v=BvKXcs-NO2o
Visit our website at https://www.geronurseprep.com/
Contact us at concne@unmc.edu for additional information or to answer any questions you might have.
Hitting Reset on Pressure Injury Prevention
The complexities of the COVID-19 public health emergency required skilled nursing facility (SNF) operations to change dramatically and often to save the lives of the most vulnerable population. Through heroic efforts, SNFs transformed clinical systems of care, sometimes in less than a day, to win the war against the pandemic.
While operations and resources shifted to battle COVID-19, unintended consequences emerged—one being greater incidence of pressure injuries. Now that the pandemic is at a turning point, facilities can start to refocus and improve this trend. This article suggests ways to reorient efforts toward preventing and managing pressure injuries.
Read the full article at https://www.providermagazine.com/Monthly-Issue/2021/July/Pages/Hitting-Reset-on-Pressure-Injury-Prevention.aspx
Careers in Aging Week will be held April 18-24, 2021
The Gerontological Society of America (GSA) hosts Careers in Aging Week every year to raise awareness about the diverse careers available in the field of aging.
People are living longer and populations are aging worldwide. The demand for professionals with expertise in aging is growing rapidly. Careers in Aging Week (CIAW) is observed every year by businesses, clinics, coalitions, organizations, universities, colleges, and other parties across the world. The goal of CIAW is to bring greater awareness and visibility to the wide-ranging career opportunities in the field of aging
For additional information and resources please go to https://www.geron.org/programs-services/careers-in-aging-week
Is your facility prepared for returning families?
If all goes well, over the next few weeks there will be an increasing number of family members visiting their loved ones in the nursing home, many for the first time in a year. Along with the joy and relief of these reunions, we can expect to observe a great deal of sadness over time lost with elders. Here are some tips on how to prepare.
Keeping Residents Active Can Forestall Falls
It is important for physicians, staff, and families to find creative ways for residents to stay on the move.
Read more at http://www.providermagazine.com/archives/2020_Archives/Pages/0620/Keeping-Residents-Active-Can-Forestall-Falls.aspx
Federal Help Falters as Nursing Homes Run Short of Protective Equipment
Around the country, nursing homes trying to protect their residents from the coronavirus eagerly await boxes of masks, eyewear and gowns promised by the federal government. But all too often the packages deliver disappointment — if they arrive at all.
Read the full article at https://www.managedhealthcareconnect.com/content/federal-help-falters-nursing-homes-run-short-protective-equipment